Polycystic Ovary Disorder (PCOD) and Polycystic Ovary Syndrome (PCOS) are among the most common hormonal conditions affecting women of reproductive age today. Despite being widely discussed, these two conditions are often confused with each other. While both affect the ovaries and can cause similar symptoms, their underlying causes and health impacts are quite different.
In this article, we’ll explore the early signs of PCOD and PCOS, their causes, risk factors, and key differences, so you can understand when to seek medical advice and how to manage your reproductive health better.
What Are PCOD and PCOS?
Although the terms are used interchangeably, PCOD and PCOS are not the same condition.
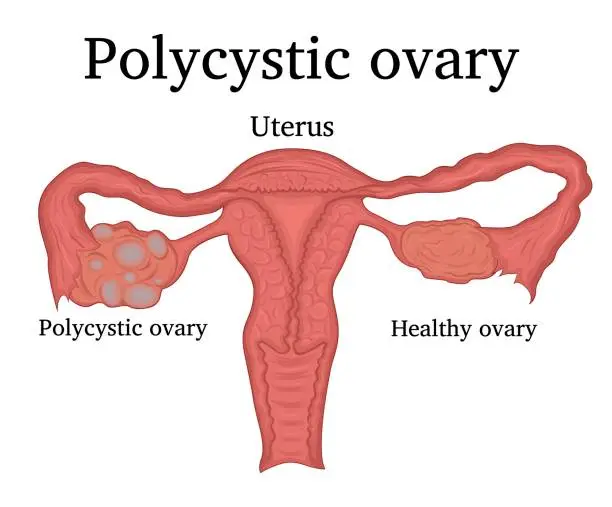
PCOD (Polycystic Ovary Disorder) refers to a condition where the ovaries release many immature or partially mature eggs that eventually become cysts. This can lead to enlarged ovaries and hormonal imbalance, but is generally less severe than PCOS.
PCOS (Polycystic Ovary Syndrome), on the other hand, is a metabolic and endocrine disorder that not only affects the ovaries but also disrupts the overall hormonal and insulin balance in the body. It can cause irregular periods, fertility problems, weight gain, and an increased risk of diabetes and heart disease.
Both conditions need medical attention, but PCOS often requires more long-term lifestyle and hormonal management.
Early Signs of PCOD and PCOS
Identifying the early signs of PCOD and PCOS can help women take timely action and prevent complications. Here are the most common symptoms to watch for:
1. Irregular or Missed Periods
One of the first warning signs of both PCOD and PCOS is irregular menstrual cycles. Women may experience delayed, infrequent, or even missed periods. In some cases, the flow may be heavier or lighter than usual.
2. Excessive Hair Growth (Hirsutism)
Due to increased levels of male hormones (androgens), women with PCOS often notice unwanted hair growth on the face, chest, abdomen, or back. This is one of the most visible signs of hormonal imbalance.
3. Acne and Oily Skin
Hormonal fluctuations can lead to acne breakouts, especially on the face, chest, and upper back. The skin may also become oily and prone to blackheads.
4. Weight Gain and Difficulty Losing Weight
Many women with PCOS or PCOD struggle with weight management. The hormonal imbalance and insulin resistance make it difficult to lose weight, even with diet and exercise.
5. Hair Thinning or Hair Loss
While some areas of the body experience excess hair growth, scalp hair may thin out or fall excessively, resembling male-pattern baldness.
6. Dark Patches on the Skin
Darkened skin, especially around the neck, groin, or underarms (a condition called acanthosis nigricans), can indicate insulin resistance—a common symptom of PCOS.
7. Mood Changes and Fatigue
Hormonal changes can affect mood and energy levels. Women may feel unusually tired, irritable, or anxious.
8. Infertility or Difficulty Conceiving
Irregular ovulation or lack of ovulation (anovulation) is a major reason many women with PCOS or PCOD find it difficult to conceive naturally.
If you notice several of these symptoms, it’s advisable to consult a gynecologist for a proper diagnosis.
Causes of PCOD and PCOS
The exact causes of PCOD and PCOS are not fully known, but research suggests they arise from a combination of genetic, hormonal, and lifestyle factors.
1. Hormonal Imbalance
An increase in male hormones (androgens) disrupts the normal menstrual cycle and prevents eggs from maturing properly. This leads to cyst formation in the ovaries.
2. Insulin Resistance
In many PCOS cases, the body’s cells do not respond properly to insulin. As a result, the pancreas produces more insulin to compensate, which can increase androgen levels and worsen symptoms.
3. Genetic Predisposition
Women with a family history of PCOS or diabetes are more likely to develop the condition. Certain genes linked to insulin resistance and hormone regulation may play a role.
4. Unhealthy Lifestyle
Poor diet, lack of physical activity, and high stress levels can contribute to weight gain and insulin resistance, worsening the symptoms of PCOD and PCOS.
5. Inflammation
Low-grade inflammation in the body is common among women with PCOS and may be linked to increased androgen production.
Risk Factors of PCOD and PCOS
While any woman can develop these conditions, some are at higher risk. The most common risk factors of PCOD and PCOS include:
- Family history of PCOS, diabetes, or obesity
- Overweight or obesity, especially around the abdomen
- Sedentary lifestyle with minimal physical activity
- Unhealthy eating habits, such as high sugar or processed food intake
- High stress levels or poor sleep quality
- Hormonal birth control misuse without medical supervision
- Early onset of menstruation (before age 11)
Understanding these risk factors can help in early detection and lifestyle modification.
Key Differences Between PCOD and PCOS
| Feature | PCOD (Polycystic Ovary Disorder) | PCOS (Polycystic Ovary Syndrome) |
| Nature | Ovarian disorder | Metabolic-hormonal syndrome |
| Cause | Due to a hormonal imbalance causing cysts | Linked to insulin resistance and hormonal dysfunction |
| Severity | Milder and often reversible | More serious and affects multiple organs |
| Fertility Impact | Usually not severe; many women conceive naturally | Often causes infertility and requires treatment |
| Weight Impact | Mild to moderate weight gain | Significant weight gain, especially around the abdomen |
| Management | Lifestyle changes and diet | Lifestyle, medication, and hormonal therapy |
While PCOD can often be managed through lifestyle modifications, PCOS may require a combination of medication, hormonal therapy, and long-term management.
How Is PCOD/PCOS Diagnosed?
Doctors typically diagnose PCOD or PCOS through:
- Medical history and symptom review
- Physical examination, including BMI and hair growth assessment
- Pelvic ultrasound to check for cysts or enlarged ovaries
- Blood tests to measure hormone levels, insulin, and glucose
Early diagnosis helps in managing symptoms effectively and preventing complications such as infertility, diabetes, and cardiovascular diseases.
Management and Treatment Options
While there is no “cure” for PCOD or PCOS, the symptoms can be effectively managed through lifestyle and medical care.
1. Lifestyle Modifications
- Healthy Diet: Include high-fiber, low-sugar foods, whole grains, fruits, and vegetables.
- Regular Exercise: Brisk walking, yoga, or strength training at least 4–5 days a week.
- Weight Management: Even a 5–10% weight loss can improve hormone balance.
- Stress Control: Meditation, mindfulness, or counselling can help reduce cortisol levels.
2. Medical Treatment
- Hormonal Therapy: Birth control pills or progesterone tablets to regulate periods.
- Insulin-Sensitizing Drugs: Such as metformin for insulin resistance.
- Fertility Medications: For women trying to conceive.
- Topical or Oral Treatments: For Acne and Hair Loss.
Always consult a qualified gynecologist or endocrinologist before starting any treatment.
When to Visit a Gynecologist
You should consult a doctor if you:
- Miss your periods for several months
- Notice excessive hair growth or severe acne
- Experience sudden weight gain or hair loss
- Are you struggling to conceive after 6–12 months of trying?
Early medical guidance can prevent long-term complications and restore hormonal balance.
Conclusion
Both PCOD and PCOS are increasingly common among women today—largely due to lifestyle changes, stress, and poor dietary habits. Recognizing the early signs of PCOD and PCOS, understanding their causes and risk factors, and seeking timely medical care can make a huge difference.
If you suspect symptoms of hormonal imbalance, visit your nearest gynecologist or a women’s health clinic for screening and personalized treatment. With the right guidance, lifestyle changes, and medical support, PCOD and PCOS can be effectively managed, allowing you to lead a healthy, balanced life.


